This story was published in partnership with The Guardian.
Introduction
Subscribe on Google | Apple Podcasts | Spotify | Amazon
Jabriel Muhammad pays up to $40 when he sees a doctor at the community health center in Jefferson County in rural southwestern Mississippi, and he goes to the center only when he is really ill. But there’s another price to pay for not having health insurance. In October, he was hit with a $1,394 hospital bill for an MRI scan to diagnose why he wasn’t breathing properly.
“We’re poor folks trying to make it as best we can,” said Muhammad, a 40-year-old self-employed carpenter and plumber. “If I make $10,000 with the work that I do in a year, that’s a nice feeling to me.”
In Mississippi, the poorest and blackest state in the U.S., single adults without children like Muhammad are not eligible for public health insurance, regardless of how little they earn each year. If he lived 30 miles west in Louisiana, across the Mississippi River, he could afford to see a doctor more often.
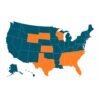
Louisiana is the only Deep South state that expanded Medicaid under the 2010 Affordable Care Act, which extended health care access for the working poor. Like Muhammad, most of the 2 million people in the U.S. without expanded coverage live in eight states in the South, where the legacy of slavery continues to shape healthcare policies, efforts to alleviate poverty and the life circumstances for Black people.
In Mississippi, 78% of the people who would become eligible for health insurance with Medicaid expansion are like Muhammad — poor adults without children.
“The denial of Medicaid coverage is scandalous,” said Don Simonton, a retired professor from Alcorn State University, a historically Black college in Mississippi. “It is so typical of the power structure of the South from slave days forward: ‘If you’re poor, you better make some money if you don’t want to die.’”
Advocates such as the Center on Budget and Policy Priorities, a think tank that supports policies to reduce poverty and inequality, say: “Many of the states that have refused expansion have a long history of policy decisions based on racist views of who deserves to get health care services.”
The pandemic and the racial justice uprising following the killings of Breonna Taylor and George Floyd last year focused the nation’s attention on health care disparities among people of color that states have allowed to fester, even as the pandemic punctuated how those disparities can be deadly.
That’s especially true in rural Black communities that lack adequate access to basic preventive health care services to treat chronic diseases. Many uninsured people avoid doctor’s visits until it’s a life-or-death scenario.
Medicaid expansion was designed to reduce racial and geographic inequities in health insurance coverage. The expansion also sought to create a national standard; however, that didn’t happen because, as in the past, some states refused to participate.
Jefferson County, once the home of thriving plantations, sits just downstream and across the Mississippi River from Madison Parish, Louisiana. Both places are named for former presidents and slave owners and are among the poorest and blackest in the country. But in Madison access to health insurance for the working poor has cut the amount of unpaid care costs from insurers and patients. This demonstrates how access to health care can change lives and reduce longstanding racial disparities.
Prior to the Affordable Care Act, more than 20% of adults younger than 65 in both counties were uninsured. Then their paths diverged. In Madison Parish, the uninsured adult population has plunged 8 percentage points since 2015, while Jefferson County stayed the same.
Medicaid expansion has extended a lifeline to some rural hospitals that have faced closures across the country. Since the major Affordable Care Act Provisions took hold in 2014, charity care and bad debt, which pose a major financial burden to hospitals, have fallen among all hospitals. (Many states pick up some of the costs, burdening state budgets.)
However, the most significant declines were in Medicaid expansion states whose costs are less than half of the costs in non-expansion states. In Louisiana, hospitals spent 8.9% of their operating expenses on debt resulting from the costs of unpaid care in 2016. But that figure declined to 5.5% in 2020. In Mississippi, however, the same debt has hovered above 7% during the same four-year period, according to data from the Centers for Medicare and Medicaid Services.
Still, beyond shoring up some rural hospitals and improving health care access, these communities face an uphill battle due to years of neglect. The pandemic has exacerbated existing problems. Unemployment is up. Fewer people are seeking primary care and treating underlying medical conditions.
Amid these challenges, there’s a deep bent toward self-reliance. By following public health guidelines, Jefferson County has done something Mississippi won’t — become the most vaccinated county in one of the least vaccinated states.

The Modern-day Slavery
Jefferson County, where Muhammad was born and raised, was once one of Mississippi’s wealthiest counties controlled by few white families until the end of slavery and the Civil War set it on a path to becoming among the nation’s poorest today. About 38% of residents live below the poverty line. Nearly 70% are on some form of government assistance. The median household income is $20,000 below the state’s.
In September, Mississippi’s state economist released a report showing that Medicaid expansion would add 11,300 jobs between 2022 and 2027, significantly reduce hospital costs for unpaid care and pay for itself for at least a decade. Governor Tate Reeves insists, nevertheless, that opting in would be bad medicine. “I firmly believe that it is not good public policy to place 300,000 additional Mississippians on government-funded health care,” Reeves, a Republican, wrote last year in his budget recommendation.
Living in a Medicaid expansion state is a protective factor for rural hospitals that have faced closures across the country. The hospitals in Jefferson County and Madison Parish are the nuclei of their communities. But the Jefferson County Hospital & Behavioral Health Unit has been limping along for years, in part because it’s being reimbursed at a rate that’s too low to cover its costs.
The jobs that would bubble up if Mississippi were to expand Medicaid could benefit Jefferson County, whose unemployment rate of 18.4% last year was the fourth-highest in the country.
Highway 61, the "Blues Highway," runs up and down western Mississippi and through Jefferson County. Lined with thick timber and comfortable homes, it's bypassed the county seat for decades.
Without the highway traffic, Fayette, like much of the county, feels apart. Main Street is a mix of empty storefronts, low-income housing, single-family homes, a bank, government buildings and a sprinkling of notable businesses, like a Muslim theatre and bakery. Around the corner, dozens of narrow, rusty trailers look like squeezed accordions.
Locals say that the only grocery store sells rotten produce. The next nearest option is 30 minutes away. “You can’t get to Natchez and so you end up buying brown meat and fruit that lasts for two days,” Pastor Tracy “Rev” Collins said.
Like Muhammad, a member of The New Nation of Islam, many here create work for themselves because there aren’t enough well-paying jobs outside of the school system, healthcare and government. The state has graded the school district an F. And people with four-year college degrees have trouble finding a job.
“I call it the modern-day slavery,” Alford Perryman, a local health insurance salesman said on a recent morning. He sat at a tall table at 61 One Stop, a gas station and community gathering space in Fayette owned by Janell Edwards and her husband. “It’s the new way to keep us from progressively moving forward at a faster pace than they are.”
Edwards hummed in agreement. “It is a big conundrum of obstacles that really comes from the same source.”
“Four hundred years,” Perryman said. “Four hundred years,” Edwards replied, “of how we came to this country and then the mentalities that were birthed out of that.”
Federalism, Racial Inequality and Medicaid
The Medicaid program was birthed in 1965, a critical year for healthcare in America and also for civil rights. The seeds of the safety net program were in civil rights legislation that sought to advance economic, legal and political rights of Black people and President Lyndon B. Johnson’s Great Society, a massive social reform initiative that sought to end poverty, among other things.
Healthcare was a critical part of combating poverty. Initially, the government had considered a federally run national healthcare program to serve vulnerable populations. But Southern politicians, who opposed civil rights legislation, shaped federal health policy. Administering Medicaid as a state-run program promised to temper their resistance to what they considered federal overreach. Medicaid has been hamstrung ever since.
During the same year in Natchez, next door to Jefferson County, the local NAACP president started his car one day and it exploded. The city’s African-American community boycotted white-owned businesses in protest and made several demands of local officials. Months later, the city surrendered.
Charles Evers came to southwest Mississippi to lead the Natchez protests. Evers had succeeded his brother, Medgar, as head of the state NAACP after a white supremacist assassinated Medgar in his driveway. Weeks before Evers arrived, a suspected Klansman shot and killed a disabled Black man on Main Street in Fayette.
When Medicaid was created, it met little fanfare because a similar, prior program had done little to address healthcare disparities, according to Jamila Michener, co-director of the Cornell Center for Health Equity at Cornell University.
“Even while recognizing the path-breaking value of Medicaid, we must concede that it has taken constant political struggle to keep the program alive,” Michener writes in her book, “Fragmented Democracy: Medicaid, Federalism and Unequal Politics.” “The political compromises spawned by that struggle have paved the way for geographic inequities.”
The Medicaid program, which matches federal dollars to state money to provide health care to the most vulnerable, is of special benefit to Mississippi. For many states, the match is roughly dollar for dollar. For every $1 Mississippi spends on Medicaid, the federal government spends $5.46, more than any other state.
Federal law mandates that states cover certain qualified, low-income groups such as families, people with disabilities, seniors, pregnant people and children. But the state ultimately decides who else is eligible, often by using a specific percentage of the official federal poverty level as a requirement.
A 2012 U.S. Supreme Court decision gave the states the option to decline to expand eligibility and the decision fell largely along partisan lines. That left what came to be called a coverage gap where some people were too poor to qualify for the health insurance subsidies the Affordable Care Act made available, but not poor enough to be covered by Medicaid under state guidelines.
The ACA provides subsidies to people whose incomes are between 100% and 400% of the federal poverty level. States that expand Medicaid cover adults with incomes up to 138% of poverty, or $30,305 for a family of three in 2021.
The American Rescue Plan Act President Joe Biden signed in March 2021 also temporarily expands the subsidies and extends them to people with incomes above 400% of poverty through next year. Mississippi is among the eight southern states, 12 in all, that continue to refuse to expand this healthcare service.
In 2016, Louisiana’s newly elected Democratic governor opted in by executive order, and since then Medicaid coverage of the adult population has increased by nearly 40%. Not so in Mississippi and the southern states that stayed out, where the proportion of the adult Medicaid population has not improved or even declined. For now, parents in Mississippi must earn less than $5,712 annually for a family of three to qualify.
"There's nothing inherently more deserving about the people in Louisiana,” Michener told Public Integrity. “We can say, 'well it's Mississippi's choice.' I think we always have to balance that logic, which is historically grounded in racism, frankly and white supremacy. I think we always have to challenge that logic and hold it up to the other things we value."
Everything ‘Revolves around the Hospital’
In Madison Parish, 46-year-old Alvin Brown risked crushing medical debt earlier this year when he found himself in the emergency room. The Medicaid program saved him from paying a whopping $9,000 hospital bill.
Brown’s ordeal began the last full week of May. "All of a sudden, I just felt bad," Brown said. His back hurt and it was painful to urinate. The next day, he visited the emergency room at Madison Parish Hospital. That’s when a doctor told Brown he was passing a kidney stone and prescribed him medication.
But two days passed and Brown was still feeling lousy. He wanted a second opinion so he tried to make an appointment with his primary care doctor located in another parish. Brown didn’t get to see his doctor. Instead medical staff at the emergency room in Richland Parish referred him to a kidney specialist. St. Francis Medical Center even further west in the city of Monroe, nearly an hour away from where he lives, admitted him.
“That was my first time ever being in the hospital,” he said about the week-long hospital stay. “I never had no [health] issues or nothing.”
It so happens that Brown was dehydrated. As a result, his kidneys began to malfunction. "It was kind of scary," said Brown, a father of a 15-year-old boy. "I don't want to be on no dialysis. It was just that I had a bad kidney."
He learned his accidental insurance, which is supplemental, had expired. A hospital employee asked if he was interested in enrolling in Medicaid, which he didn’t know he qualified for. The coverage kicked in just in time to pay $7,000 of his $9,000 hospital bill. It would have been "rough" to pay off the debt without it, he admitted.
Brown, who stocks liquor and wine for retail outlets, has a $28,000 annual household income for a family of three. That puts him just under the threshold of earning 138% of the federal poverty level to qualify for Medicaid coverage. "You never know what life throws at you so always be prepared," he said. That debt could have turned into care the hospital wasn’t paid for.
Since Louisiana expanded Medicaid in 2016, uncompensated care costs dropped 55% among the state’s rural hospitals, according to a study in the March 2021 issue of Health Affairs. “In this one dimension, compared to hospitals in non-expansion states, hospitals in Louisiana appear to be much better off after Medicaid expansion,” said lead author, Tulane University Professor Kevin Callison.
Hospitals that serve large numbers of low-income patients like Brown receive Disproportionate Share Payments, federal funds with a state match that help to offset unpaid patient or insurer costs. These payments are a larger proportion of Louisiana's Medicaid budget relative to most states. “If they did away with the supplemental payments, eventually a place like this would close,” said Madison Parish Hospital CEO Ted Topolewski.
Sitting in his basement office, Topolewski rattles off the hospital’s ailments: a shot roof, fire partitions that don't meet code, asbestos in electrical cabinets. In Madison Parish, local and hospital leaders are building a new facility that they hope will mean people won’t have to travel 20 or 30 miles to specialty clinics that treat conditions like diabetes or cancer.
Some residents question whether the new hospital can draw qualified providers given the parish, rolling flat land dotted with farms, lacks jobs and recreational activities. They would have preferred local leaders to prioritize investments in clean water before a new hospital. Residents like Latrice Dismuke, a 41-year-old native of Tallulah, the Madison Parish seat, says that there are times when she runs water to take a bath, and “you're looking at water that looks like tea.”
Back in Mississippi, Jefferson County Hospital & Behavioral Health Unit has been limping along for years, in part because it’s being reimbursed at a rate that’s too low to cover its costs. But it’s also been mired in leadership turnover, according to county leaders. Hospital and county leaders say it’s faced high labor costs, few specialists and a lack of equipment that can delay access to emergency care. All this on top of declining reimbursements, and therefore, increasing costs.
Medicaid expansion would help more people receive preventative healthcare services, so that they could manage their chronic conditions and avoid emergency room visits, said Mike Harrell, interim hospital administrator.
“Our hospital had been for a long time one of the biggest concerns in the community,” said Anthony “Bruce” Walton, president of the Jefferson County Board of Supervisors. “Because if we lost our hospital, then it’s like a trickle-down effect. We can’t have our prison, our schools. Everything that we have in our small community pretty much revolves around the hospital.”
A Future We Can Control
Charles Evers became mayor of Fayette in 1969. His tenure drew some industry to Jefferson County and helped launch the local community health center, among the pioneers in the movement to provide free and low-cost healthcare to indigent populations. (It was initially named for Medgar.)
Evers’ tenure, though — four nonconsecutive terms through 1989 — coincided with white flight.
“Jefferson County still suffers a bit from that, not because it doesn’t have white people, they’re not actually necessary, but because they took with them their backgrounds and their skill sets and their wealth,” said Simonton, the retired Alcorn State University professor.









At any time of day, locals cycle in and out of 61 One Stop, the part-convenience store, part-town square along Highway 61 in southwest Mississippi. “We’re not successful because we don’t have the tenacity or the determination,” Perryman said. “We’re not successful because we don’t have people in place that are vouching for us.”
Locals dutifully wear masks when outside pumping gas or inside local businesses. Eight miles north of Fayette, Arthur Davis, owner of the Old Country Store in Lorman, tells patrons to wash their hands as soon as they come in. Davis says self-protection measures like the vaccine and mask mandates work here because Black folks are the majority and in power.
“We’re not stuck with that stupid stuff,” said Davis, 74.
Davis, though, waves off notions that Jefferson County lacks local or state power. His signature fried chicken draws a largely white clientele and a loyal Black following. Pressing beyond symbols of white supremacy, he sells Confederate flag head scarves for a $22.95 profit because "we can use this as a tool."
Through their work building up Main Street in Fayette, the New Nation of Islam, a Black nationalist group that advocates for self-empowerment, is taking a different, albeit autonomous approach. This tight-knit community supports projects like a K-12 school tucked away on a windy two-lane road in an unincorporated area known as Red Lick. Muhammad, a Muslim whose friends call him brother, is working on his biggest carpentry project to date — a furniture store in the old cleaners building on Main Street in Fayette.
“The best future that you have is the one that you can control,” said the community’s spiritual leader, whose followers call him Son of Man. He envisions Main Street as a “beautiful, thriving Black community that will be a model for our people, all over the earth.”
Muhammad and other community members say the redevelopment work is possible because they make charitable contributions to Son of Man. The members of the group live and work cooperatively. That means Son of Man is helping Muhammad pay off his hospital bill — and filling a healthcare gap left by the state of Mississippi.
When it comes to healthcare access or affordability, Son of Man says, “Whatever my followers need, they get.”
Muhammad is grateful, and is paying off the $1,394 bill bit by bit. “It hurts my pocket a little because that's a good little piece of change for somebody who doesn’t make money every day.”
April Simpson is a senior reporter at the Center for Public Integrity. She can be reached at asimpson@publicintegrity.org. Follow her on Twitter @aprilleticia.
Mc Nelly Torres edited this project.
Janeen Jones designed the pages for this project.
Alex Eichenstein wrote the audience engagement strategy.
Help support this work
Public Integrity doesn’t have paywalls and doesn’t accept advertising so that our investigative reporting can have the widest possible impact on addressing inequality in the U.S. Our work is possible thanks to support from people like you. Donate now.
Read more in Inequality, Opportunity and Poverty
Inequality, Opportunity and Poverty
These books tackled inequality in 2021
A year of deep looks at discriminatory systems in government, education, policing, poverty and media.
Inequality, Opportunity and Poverty
Carol Anderson: The Second Amendment is anti-Black
The Kyle Rittenhouse verdict and Ahmaud Arbery trial illustrate the Second Amendment’s racist roots, says author Carol Anderson.






Join the conversation
Show Comments